Same-day Appointments Book Online
Call to book 201.523.9590
Same-day Appointments Book Online
Call to book 201.523.9590
 Same-day Appointments Book Online
Call to book 201.523.9590
Same-day Appointments Book Online
Call to book 201.523.9590
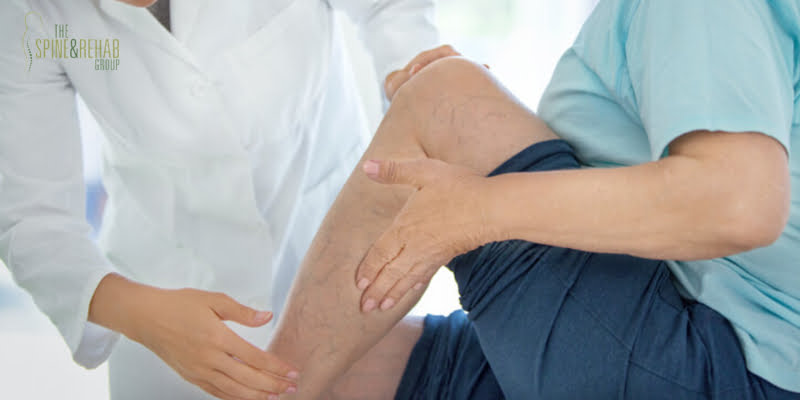
The nervous system is one of the most critical parts of your body, and a large reason it functions so well is because of the spine. The spine has plenty of crucial functions like supporting the head and giving structure to the body, but it’s also the center of the entire nervous system. With all the different areas connected to the spine, it’s not uncommon for any kind of body pain to be linked to something going wrong with it. So when do you know if your leg pain is caused by spinal stenosis? Typically, only a professional consultation can properly give a diagnosis. However, there are a few things that you can rule out on your own to give the doctor better information when you go for an appointment.
Spinal stenosis is a condition where the gaps in the spinal column narrows, which compresses the spinal cord and other nerve endings. While it can occur anywhere in the spine, it’s more common along the lower back or the lumbar region. The reason spinal stenosis can cause so much pain is that the nerves need the gaps between vertebrae to branch out to areas like the legs and lower back. When your spine narrows, these nerves effectively get pinched by the pressure. Adding in factors like the overall weight supported by the spine, spinal stenosis can cause a lot of frequent flashes of pain that can become chronic with time.
So when is leg pain linked to spinal stenosis? Here are some things that you should keep in mind:
Symptoms of spinal stenosis can differ depending on the progression of the condition, but most patients will usually experience the following:
It’s important to remember that these symptoms rarely present themselves all at once, and can be easily mis-attributed to something else. So it’s crucial to have yourself checked out by a doctor if you have any of these symptoms. Because spinal stenosis gets worse over time, catching it early and starting treatment options immediately is the best way to manage it.
While any disease or condition that can affect the spine can trigger spinal stenosis, there are a few health conditions that make it more likely to occur:
But by far, the biggest culprit behind most cases of spinal stenosis is aging. Because the body breaks down and becomes more fragile as you get older, you’re more likely to get spinal stenosis simply because your body can’t carry your weight anymore. Other factors like being overweight and lifestyle can play a role but are not usually the primary cause except in very rare circumstances.
If it is spinal stenosis, your doctor will prescribe one or more of the following treatments:
Medication is one of the first treatment options for spinal stenosis, mostly because it’s a non-invasive method that doesn’t require a lot of work on part of the patient. One of the most-used treatments is cortisone injections directly into the spinal column, as that can reduce most pain and inflammation that puts pressure on the nerves.
You may also take nonsteroidal anti-inflammatory drugs (NSAIDs) for the pain. However, the use of these medications should only be upon the advice of your doctor, since they can interfere with other medication or treatment options to relieve your pain. In particular, people who are scheduled for regular epidural steroid injections should be very careful with using medication.
Another preferred treatment option for spinal stenosis is physical therapy. This kind of treatment is especially effective if leg and lower back pain has become chronic since it can help condition the body to support itself better while it moves. Most physical therapy sessions will last for a few months if spinal stenosis is diagnosed early, and can be complemented by physical exercises at home. Therapy will often focus on strengthening the muscle groups of the leg and lower back to help support the spine better. However, flexibility exercises can also be integrated with the treatment regimen so the gaps between the spine loosen up.
Finally, in extreme cases where spinal stenosis has already affected functions like motor control and bowel movements, surgery is required. There are several types of spinal surgery that doctors can use to treat spinal stenosis, and the prognosis for those who undergo the procedure is positive. However, it should be noted that surgery is the last resort for spinal stenosis.
Because it usually involves direct work on the spinal column, the procedure carries more risk – and cost – compared to other treatment methods. This is also another important reason doctors prefer catching spinal stenosis before it progresses too far. Again, spinal stenosis can be a cause of leg pain, but the only way to make sure is to consult your doctor. Any self-diagnosis or self-medication should be avoided.
Related article: How To Prevent Spinal Stenosis From Getting Worse?
If none of the symptoms of spinal stenosis correspond to your leg pain, it could be caused by something else. Here are some of the most frequent culprits of leg pain, and how you can identify them:
Peripheral artery disease (PAD) occurs when the blood vessels in your body narrow and constrict. It usually occurs with people who also have type-2 diabetes and is often detected when it causes acute or chronic pain in the legs and feet.
PAD is caused by a buildup of fat or plaque deposits in your blood vessels, which restricts their ability to bring blood, oxygen, and nutrients to the extremities of your body. One of the earliest warning signs of this condition is a feeling of pain, numbness, or tingling in the legs and feet. Other symptoms may also include injuries like sores or bruises along your legs that don’t heal quickly.
While a slipped or ruptured disc can trigger spinal stenosis, it’s also likely to trigger leg pain on its own. Most of the time, these usually occur because of active injury to the spinal column. Herniated and bulging discs are often characterized by chronic pain and discomfort radiating from the spinal column to the affected joint, though it’s possible to have no symptoms at all.
If you have a herniated or bulging disc, you must seek treatment immediately to prevent it from developing into something more serious. Because most of the nerves in the body congregate at the spine, any bulging or slipped discs will most likely affect a lot of nerves.
One straightforward explanation for leg pain is if your leg has been injured. This is most commonly caused by a strain or a sprain which can trigger pain, cramps, and numbness in the legs immediately after it happens. In most cases, home remedies and basic medical attention can address the issue and remove the pain after a while.
However, if the pain returns after the injury have already been treated, some nerves or major muscle groups have likely been affected. This is a more serious issue that requires immediate medical diagnosis or treatment. Areas like the arm and leg are particularly concerning to doctors, since they can be a sign of torn tendons or incorrectly set bones.
Gout is caused by the formation of small crystals around the body’s joints, which make them swell up and pinch on any nerves in the area. It usually occurs on the extremities like the knees, feet, and ankles, though it can technically affect any joint in the body. It’s caused by an excess of uric acid in the blood, which can be triggered by diet, diabetes, or genetics.
Symptoms of gout often include painful swelling of the joint, red skin over the affected area, and tenderness. The pain associated with gout often “flares” in sudden attacks, which can radiate from the joint towards the rest of the limb. Treatment of gout is usually enough to make this pain subside and make further pain more manageable.
Deep vein thrombosis (or DVT) occurs when a clot forms inside a blood vessel located further below your skin. It usually occurs in areas like the thighs and the legs, but it can technically develop in any blood vessel that clots. Causes can range from injury, medication, lifestyle, and even previous surgery near the affected area.
Symptoms of DVT include swelling, cramping, increased temperatures at specific spots on the leg, or discoloration of the skin. These symptoms may appear gradually or all at once, with some people not experiencing symptoms at all. In severe cases, DVT can only be diagnosed once it’s progressed to a pulmonary embolism, or when the clot has moved the lung.
With all these different causes of leg pain, always check in with your doctor if you experience leg pain that can’t be easily explained, lasts for an unusually long time, or you experience frequently even with home care. Most of these conditions can be diagnosed with an MRI or a CT scan. Alternatively, frequent physical exams and routine checkups can also help with screening.
Read more: Why Does Spinal Stenosis Make You Tired?
Instances of leg pain may not always mean spinal stenosis, but it’s best to have it diagnosed properly, especially if you’re older. Any persistent leg pain is usually one of the first symptoms of some serious diseases or disorders and is crucial for early detection of these conditions. And while it may be tempting to manage these symptoms of leg pain at home, only do this if you’ve been cleared by your doctor.
With years of experience in helping our patients with their spinal health, we at The Spine And Rehab Group pride ourselves on providing accessible, reliable, and personalized care. We can quickly diagnose and evaluate any kind of pain that you might experience, and start you on immediate treatment. If you’re experiencing any pain and would like to get checked out, visit one of our New York and New Jersey clinics today.